
The Biology of Anxiety
The Autonomic Nervous System:
Anxiety disorders are complex conditions influenced by a variety of biological, psychological, and environmental factors. The biological underpinnings of anxiety disorders involve several interconnected systems and mechanisms.
The human nervous system automatically regulates involuntary body functions and consists of two main branches:
Sympathetic Nervous System: Activates the ‘fight or flight’ response, leading to increased heart rate, blood pressure, and rapid breathing.
Parasympathetic Nervous System: Promotes the ‘rest and digest’ response. Chronic activation of the sympathetic system can lead to imbalances.
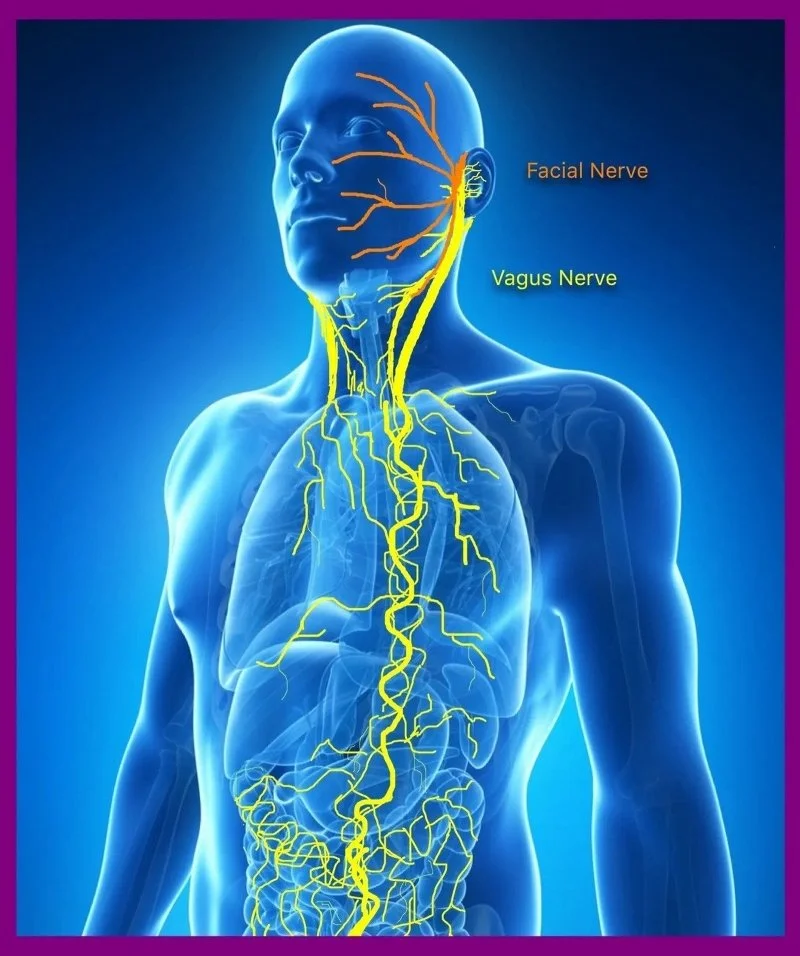
Chronic stress or trauma excessively activates the sympathetic branch, which can lead to system imbalances. The Vagus nerve is the primary control nerve for the parasympathetic system. Strengthening the vagus nerve can counteract overactivation of the sympathetic system and bring you back into balance.
Anxiety is about the brain’s response to perceived threats. Advanced imaging techniques like functional magnetic resonance imaging (fMRI) allow scientists to observe this response in real time, revealing three key brain networks that tend to malfunction in people who struggle with anxiety.
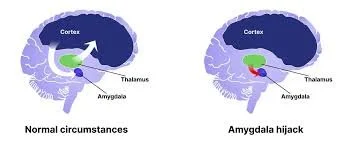
The first is the salience network, which includes the amygdala (fight-or-flight), an almond-shaped region deep in the brain that detects emotionally charged or threatening events. This is the area in the brain that determines saliency of the threat and activates the autonomic nervous system.
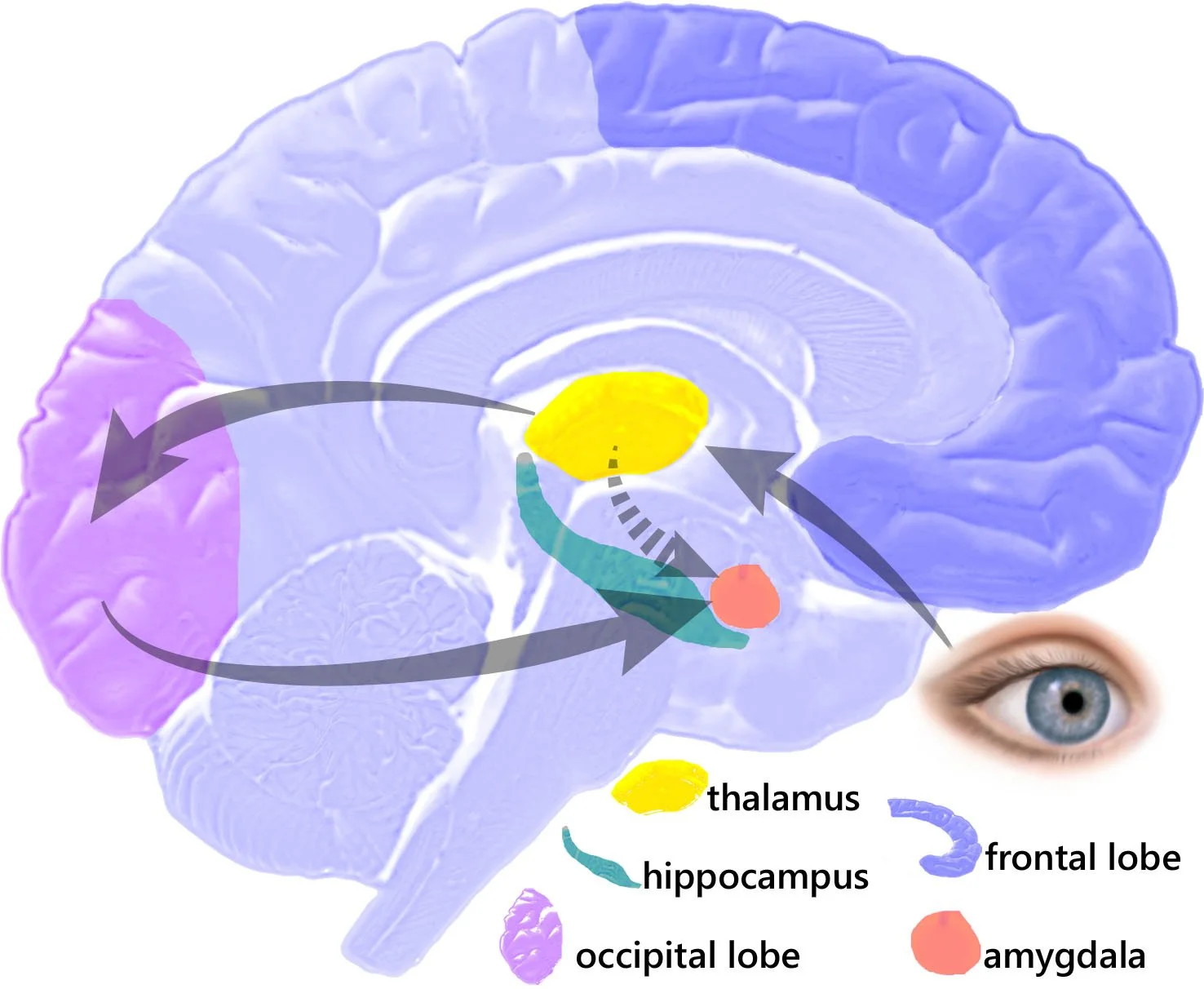
The second is the executive control network (attention), involving regions such as the middle frontal gyrus, which supports focus, planning, and emotional regulation.
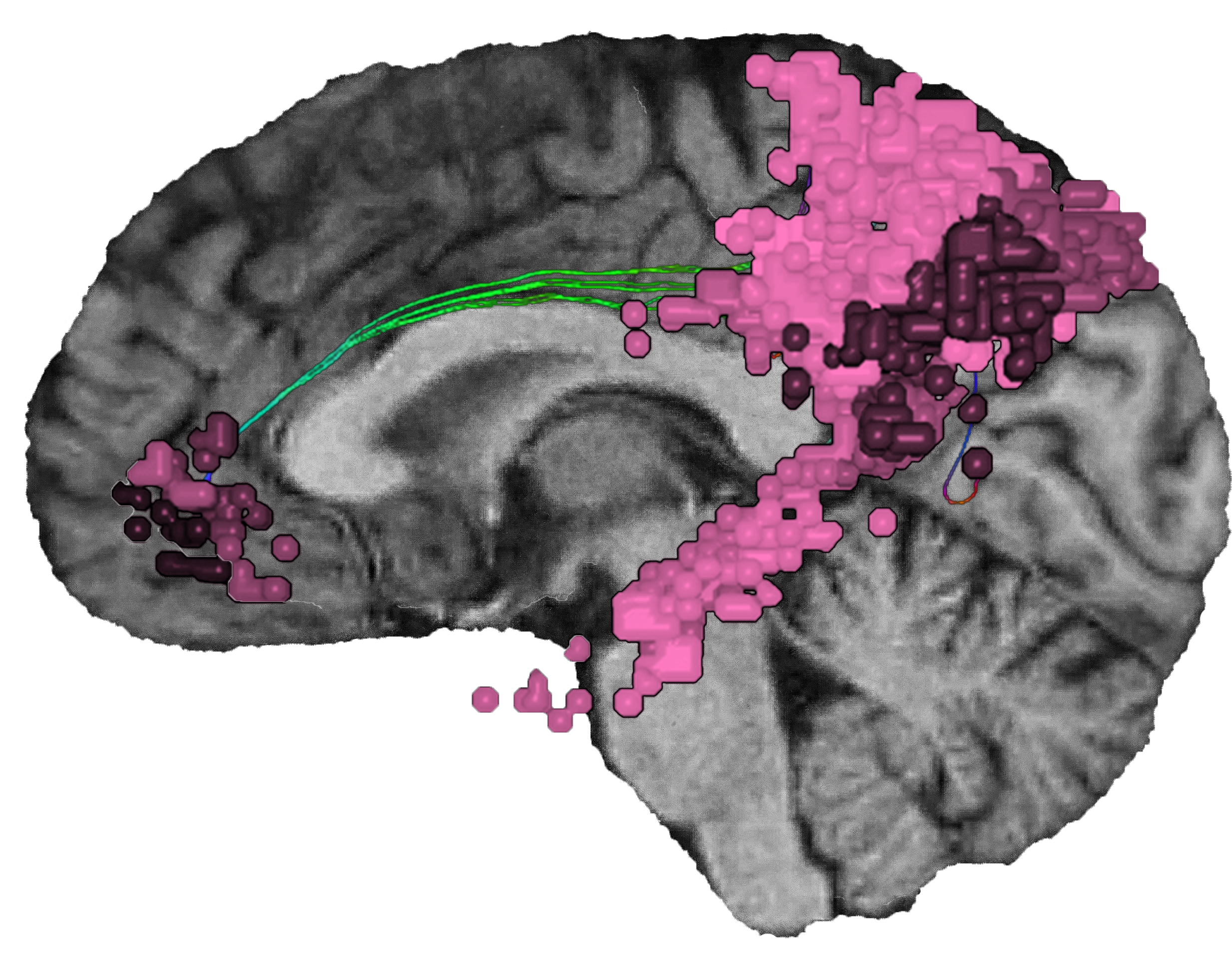
The third is the default mode network, which includes areas like the precuneus near the brain’s center and becomes active during self-reflection or when the mind wanders.
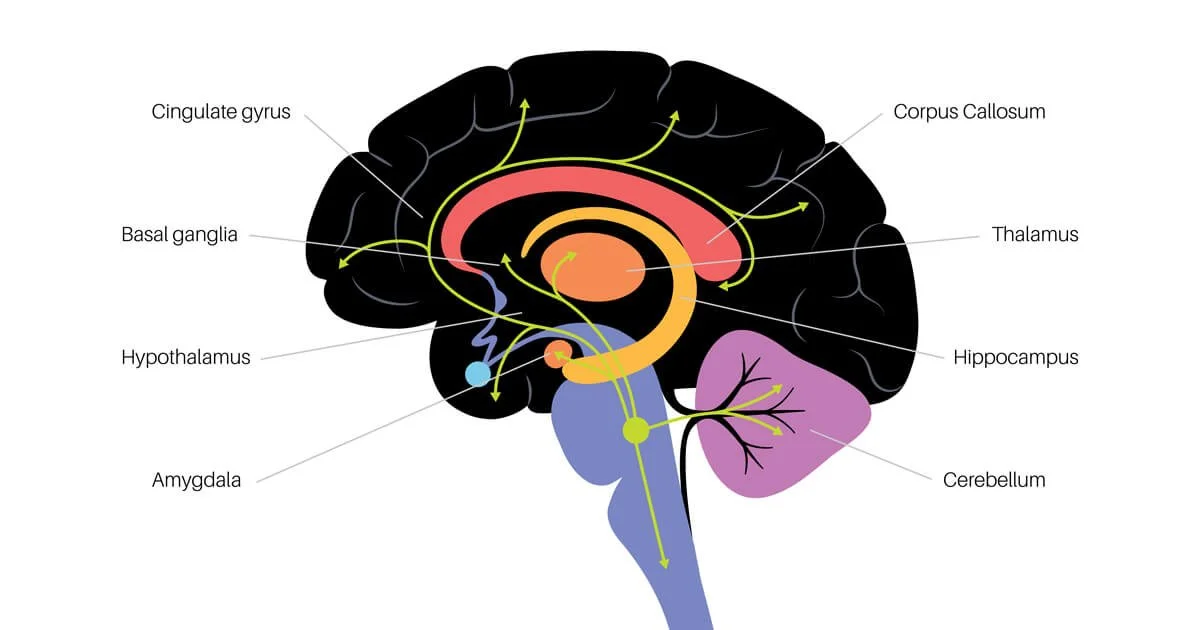
In a healthy brain, these networks shift in and out of prominence depending on what matters most at any given moment. For example, the default mode network is active during reminiscing, helping process memories, while the salience network might activate in response to an unexpected loud noise but otherwise remains in the background. These brain regions control the Central Nervous System, including the sympathetic system and the parasympathetic system, which work together to keep the brain and body in tune and functioning properly.

Understanding the Vagus Nerve
The Vagus Nerve: Functions, Stimulation Techniques, and Health Implications
The vagus nerve is one of twelve cranial nerves that connect the brain and body, extending from the brainstem to the gut. As a critical part of the parasympathetic nervous system, it helps regulate resting heart rate, breathing, and digestion, distinguishing it from the sympathetic nervous system, which is responsible for the fight-or-flight response. The vagus nerve is central to unlocking the body's relaxation response and, according to recent research, also helps modulate inflammation—a factor involved in nearly all chronic diseases, including those affecting cognition.
Vagus Nerve Dysfunction and Its Symptoms
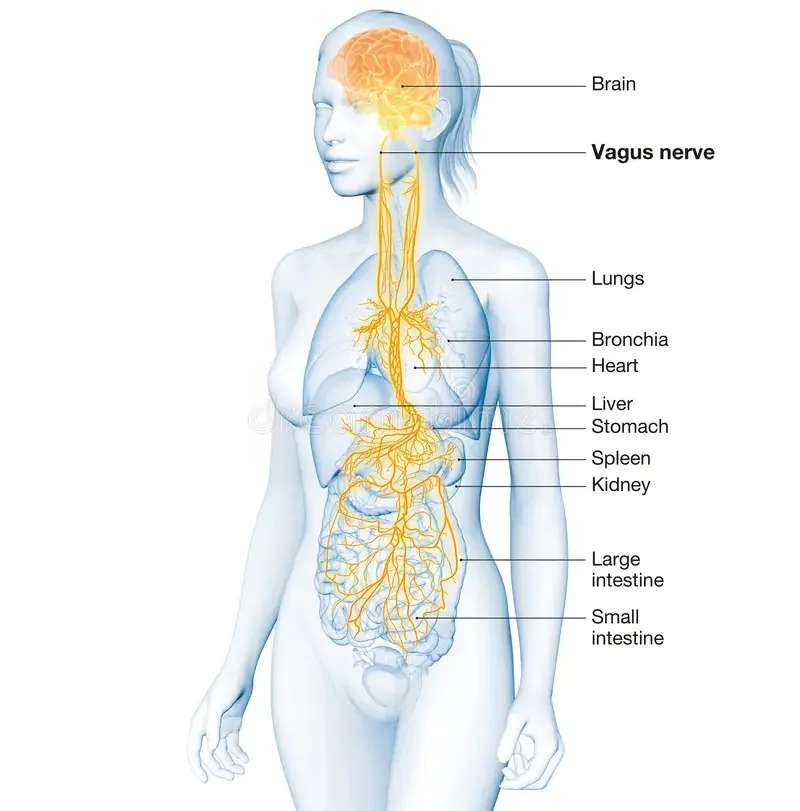
Symptoms of vagus nerve dysfunction are varied and can affect multiple systems of the body. Digestive issues may include bloating, reflux, and constipation. Cardiovascular symptoms can present as palpitations or low blood pressure. Other possible signs are hoarseness, loss of gag reflex, anxiety, depression, brain fog, fatigue, and chronic inflammation. Key indicators of vagal dysfunction include trouble swallowing, dizziness, chronic fatigue, and irregularities in heart rate or blood pressure—often resulting from impaired signaling to organs such as the gut, heart, and lungs.
The vagus nerve can also play a role in headaches, particularly migraines, cluster headaches, and cervicogenic headaches (a type of secondary headache where pain originates from the neck (cervical spine) due to an injury, poor posture, or underlying condition like arthritis, causing referred pain to the head, often on one side, with symptoms like neck stiffness and limited movement). These headaches may be caused by irritation, compression, or dysfunction of the vagus nerve, which can disrupt autonomic balance and control of inflammation. Factors such as neck trauma, spine degeneration, or chronic stress can impair vagal tone, increasing pain signals and headache frequency and intensity.
Vagus Nerve Stimulation
The FDA has approved devices that use electrical impulses to stimulate the vagus nerve for treating specific conditions such as epilepsy, depression, and migraines. Research has also shown that stimulating the vagus nerve may support brain function, even in people without underlying health conditions. Activities commonly associated with calmness—such as deep breathing, meditation, massage, and even awe—have been shown to increase vagus nerve activity and positively affect the brain. Furthermore, practices such as meditation, mindfulness, listening to music, singing, and laughter, which stimulate the vagus nerve, are also linked to a reduced risk of cognitive impairment. However, the mechanisms behind these effects are still being investigated.
Natural Ways to Stimulate the Vagus Nerve
Like muscles, nerves require activity to function optimally. Although many people do not focus on vagal nerve stimulation in their daily lives, there are several simple techniques to activate this nerve without specialized equipment. These exercises may yield significant health benefits, potentially as impactful as vigorous cardio training.
Breathing Exercises:

Slow, deep belly breathing is an effective way to stimulate the vagus nerve, as it shifts attention away from stressful thoughts and towards the rhythm of the breath. One technique involves inhaling through the nose for a count of six and exhaling through the mouth for a count of eight, watching the belly expand and contract. Practicing deep breathing for just a few minutes can keep the vagus nerve active. There are many other techniques, such as box breathing, alternating nostril breathing, double inhale, and diaphragmatic breathing.
The ancient methods for stimulating the parasympathetic nervous system include abdominal breathing and extended exhalation. Gradually increasing the depth and duration of breaths allows the body to adjust naturally. However, individuals with heart or lung diseases should consult a medical specialist before attempting these techniques.
Meditation and Mindfulness

Meditation activates the vagus nerve and calms the network of nerves that regulate various physiological processes. Not only does meditation help lower heart rate and blood pressure, but it also reduces the risk of cognitive decline and neurodegenerative disease. Mindfulness meditation, which includes pausing to notice the surroundings and breathing, can be particularly beneficial.
Loving-kindness meditation, which involves generating compassionate thoughts toward oneself and others, has been shown to increase vagus nerve activity. This form of meditation can be practiced by sitting comfortably, focusing on the breath, and mentally repeating mantras such as "May I be happy" and "May my coworkers be healthy and strong."
Laughter and Social Connection

Laughter is one of the most enjoyable ways to stimulate the vagus nerve. Watching a funny show or movie, especially with others, provides health benefits such as increased circulation, lowered blood pressure, and the release of beneficial chemicals for the cardiovascular system. Socializing with people who evoke positive emotions also enhances vagal tone, promoting stronger relationships and greater vagus nerve stimulation.
Massage and Physical Touch
Gentle massages, especially of the neck, shoulders, and feet, support vagus nerve stimulation and overall relaxation. Foot reflexology and craniosacral therapy are also beneficial. However, deep tissue or painful massage should be avoided, as it may trigger a stress response. Acupuncture—particularly when performed on the ear—can further enhance vagal activity.
Vocal Exercises: Humming, Singing, and Gargling
Singing loudly, humming, and gargling water can all stimulate the vagus nerve by exercising the vocal cords and throat muscles. These activities can also release oxytocin, fostering feelings of joy and well-being. If singing loudly is not possible, even gentle humming or gargling can be effective.
Additionally, maintaining a calm, even tone or listening to soothing voices can help soothe the body by stimulating the vagus nerve and triggering oxytocin release.
Physical Activity and Exercise

Exercise increases blood flow to the brain, stimulates the development of new neural pathways, enhances connectivity, and activates the vagus nerve. Endurance activities such as jogging, cycling, and swimming, as well as interval training, are particularly effective. Regular exercise can outperform medication for conditions like depression, anxiety, and memory loss.
Yoga (at least 90 minutes per week), tai chi, and qi gong are gentle forms of exercise that also stimulate the vagus nerve. Moderate to intense exercise, performed four times a week, provides additional benefits for mental health and vagal activation.
Experiencing Awe and Inspiration

Engaging in activities that inspire awe—such as spending time in nature, listening to inspiring music, or cultivating meaningful relationships—can activate the vagus nerve. Such experiences can lower blood pressure, inhibit the stress response, reduce inflammation, improve heart rate variability, reduce pain, and enhance sleep and mood.
Progressive Muscle Relaxation

Progressive muscle relaxation, which involves systematically tensing and relaxing muscle groups from the feet to the head, is an effective way to reduce anxiety and stimulate the vagus nerve. This practice should be performed in a quiet, comfortable environment, with attention to breathing.
Cold Exposure

Brief exposure to cold temperatures, such as taking cold showers, splashing cold water on the face, or even spending time outside in cold weather, can stimulate the vagus nerve and reduce the body's stress response. Initially, the sympathetic nervous system is activated, but as the body adapts, the parasympathetic system (and thus the vagus nerve) becomes more active.
Medical and Dietary Approaches

In some cases, medical interventions such as the implantation of a programmable pulse generator device may be recommended, particularly for individuals with epilepsy or treatment-resistant depression. These devices deliver electrical impulses to the vagus nerve and are generally considered safe, though side effects may include voice changes, throat pain, cough, headache, chest pain, or skin tingling. Noninvasive devices are also available and are becoming more popular.
Dietary strategies include increasing intake of probiotics such as Lactobacillus rhamnosus and Bifidobacterium longum, as well as omega-3 fatty acids (commonly found in fish). These supplements may influence vagal activity and mental health, although more research is needed to confirm their effectiveness in humans. Eliminating sugar, caffeine, and alcohol from the diet, and practicing intermittent fasting (when appropriate), may further support vagal tone and overall health.
Vagal Tone, Mental Health and Cognitive Functioning

Vagal tone significantly influences mental health, particularly in terms of mood regulation, stress resilience, and cognitive performance. High vagal tone promotes relaxation and faster recovery from stress, while low vagal tone is linked to increased stress reactivity, anxiety, and depression. Vagus nerve activity is also associated with cognitive functions such as attention, memory, and decision-making.
Vagus Nerve Function and Health Implications
Immune System Regulation
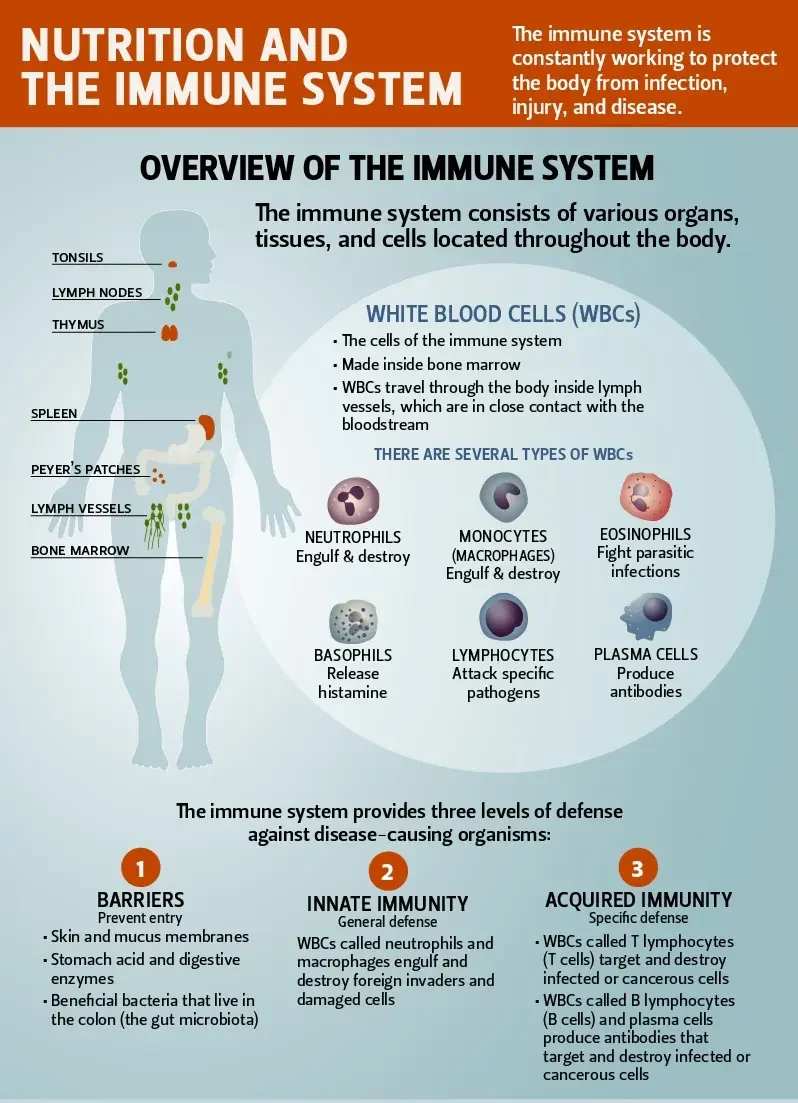
By modulating inflammation, the vagus nerve plays a vital role in preventing excessive inflammation and supporting immune health. Chronic inflammation is a common factor in many diseases, including autoimmune and neurodegenerative disorders.
Digestive Health
The vagus nerve regulates digestive processes by controlling the release of digestive enzymes, gastric acid, and bile, and by coordinating the movement of food through the digestive tract. Impaired vagal function can contribute to gastrointestinal issues such as acid reflux, gastroparesis, and irritable bowel syndrome.
Cardiovascular Health

The vagus nerve is essential for regulating heart rate and blood pressure. High vagal tone is associated with lower resting heart rate, reduced blood pressure, and increased heart rate variability (HRV), all of which indicate a healthy autonomic balance.
Enhancing Vagal Tone:

Myths and Facts About the Vagus Nerve Reset
While massage therapy and certain supplements (such as omega-3 fatty acids and probiotics) have been promoted as ways to "reset" the vagus nerve, there is limited research supporting these claims. Massage can provide general relaxation, but direct, strong, or prolonged stimulation of the vagus nerve through physical pressure is not recommended.
Conclusion
The vagus nerve is a crucial component of the nervous system, influencing both physical and mental health by regulating heart rate, digestion, inflammation, and mood. Understanding its functions and exploring strategies to enhance vagal tone can help support overall well-being and improve quality of life.



The first system, often referred to as the "rest and digest" state, is associated with feelings of safety. This green or safe zone supports social engagement, compassion, clear thinking, calmness, and overall bodily regulation. Serving as the foundation for both mental and physical health, this is the state where individuals thrive and ideally remain. This is when the parasympathetic system is in Vagal tone.
Polyvagal Theory
Introduction to Polyvagal Theory
Developed by Dr. Stephen Porges, Polyvagal Theory offers a comprehensive understanding of how our nervous system responds to safety and threat. Drawing from his work, Our Polyvagal World, How Safety and Trauma Change Us, Dr. Porges explains that the nervous system consists of three primary states, rather than just two as previously thought.
The Three Primary Nervous System States
The Green Zone: Safety and Social Engagement
The Yellow Zone: Fight-Flight Response

The second system, known as the yellow zone, represents the traditional sympathetic response. This state is marked by fight-or-flight reactions, panic, restlessness, reactivity, rage, and anxiety. It becomes activated when a person perceives a threat, preparing the body to respond to potential danger. Your parasympathetic system is inactive or less active when the sympathetic branch is active.
Automatic Responses and Defense Strategies
When faced with perceived threats, the body responds automatically and viscerally—what Dr. Porges describes as neuroception—before conscious awareness sets in, natural defense strategies, such as sympathetic arousal and vagus-nerve shutdown, as well as other possible responses like fawning and appeasement, emerge as natural reactions to danger.
Dominance of Nervous System States
At any given moment, one of these three systems is primarily in control, influenced by our internal sense of safety or threat—regardless of whether the threat is real. The remaining systems operate in the background, offering support. When in the green zone, individuals are more capable of learning, remembering, and interacting with others. However, when stress or overwhelm sets in, the yellow or red zones can take over, impairing optimal functioning in certain respects, as the body prioritizes survival. This helps to explain how anxiety can quickly take over your system, and you cannot control this with your thoughts.
The Red Zone: Shutdown and Dissociation

The third system, referred to as the red zone, involves shutdown or dissociative responses. Individuals experiencing this state may feel numb, hopeless, helpless, or unable to engage socially. This zone is the body's way of coping during moments of severe danger or life-threatening situations, leading to reactions such as blacking out or emotional numbing. This is (according to this theory) due to overactivation of the vagus system, which has a downregulatory effect, shutting down the body's major organs and functions. This could potentially save your life in an extreme emergency, for example, if you are bleeding out, shutting down your heart could buy you more time, or becoming paralyzed might save you from a predator.
Video: Introduction to Polyvagal Theory
Polyvagal Theory and Trauma Responses
Immobilization and the Red Zone
Polyvagal Theory enhances our understanding of how the nervous system copes with severe trauma or life-threatening situations. The third branch of this system is linked to immobilization, numbness, and an ancient state of paralysis. While this shutdown response is most evident in life-threatening circumstances, it can also occur in many other situations where a person feels overwhelmed. In the aftermath of trauma, individuals may withdraw or find it difficult to manage certain aspects of daily life. Activities and decisions that once felt routine may become challenging or impossible. This shift is a direct result of trauma, often leaving individuals feeling stuck or unable to progress. When threatened, the sympathetic nervous system may trigger hyperarousal (the fight-or-flight reaction), or the dorsal vagus nerve may activate the shutdown response. Both scenarios elicit a range of emotional experiences, such as anxiety, fear, hatred, and anger. If regulation is achieved, the nervous system can return to the green zone, characterized by calmness, safety, and openness to social engagement.
Navigating and Regulating Nervous System States
All three nervous system states are necessary for survival, yet transitioning back to the green or safe state after the red zone is engaged can be particularly challenging. Developing awareness of these systems allows for greater insight into our internal experiences. Remaining stuck in the yellow (fight-or-flight) or red (shutdown) zones often results in significant discomfort, leading to a desire for relief. In response, many individuals may turn to addictive behaviors such as substance use, overeating, overspending, codependent relationships, sexual addictions, or persistent negative thoughts to cope with the distress. Gaining an understanding of the nervous system’s workings can be instrumental in creating a safe environment to learn healthier coping strategies, ultimately helping to avoid these maladaptive patterns.
